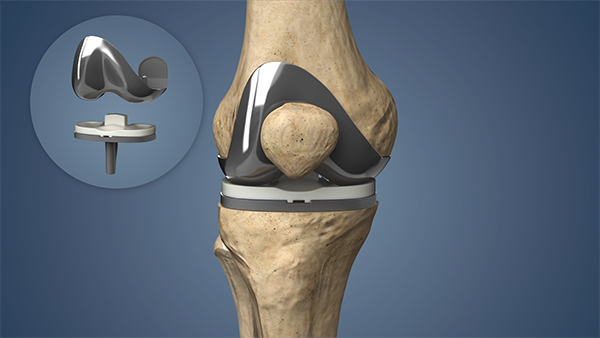
The conversation before a knee replacement tends to focus heavily on the procedure itself — the implant, the incision, the hospital stay, the rehabilitation timeline. What is discussed far less thoroughly is the long-term reality of living with a replaced knee: what it will feel like five years later, what activities will be possible and what will not, what determines whether the implant lasts 15 years or 25, and what happens if it eventually fails. As a joint replacement surgeon in Kharadi, Dr. Mandar Puranik at orthoclinicpune.com believes that informed patients make better surgical decisions and have better long-term outcomes.
This blog is not intended to discourage anyone from a knee replacement that they genuinely need. Knee replacement is one of the most successful and life-changing operations in orthopaedic surgery. It reliably relieves severe arthritic pain and restores meaningful function in the vast majority of patients. The goal here is to give patients the complete picture — the things that are sometimes glossed over in a busy consultation — so that expectations are realistic and decisions are truly informed. Find Dr. Mandar Puranik on Google to discuss your specific situation.
Ready to consult? Book An Appointment with Dr. Mandar Puranik today.
How Long Does a Knee Replacement Actually Last?
The standard answer given to patients is that a knee replacement lasts 15 to 20 years. This is broadly accurate but significantly oversimplified. Modern data from national joint registries — databases that track the outcomes of every joint replacement performed in a country — shows that survival rates for contemporary knee implants at 15 years are above 90 percent in appropriately selected patients. At 20 years, the survival rate remains above 80 percent.
However, these averages conceal important variability. Some implants last more than 30 years. Others fail within five. The factors that determine where on this spectrum your implant falls are not random — they are largely predictable and most of them are known before the surgery takes place.
What Actually Determines How Long a Knee Replacement Lasts
1. Patient Age at the Time of Surgery
This is the factor patients most commonly misunderstand. A younger patient at the time of surgery has a higher lifetime risk of requiring a revision (repeat replacement) simply because they will live longer. A 55-year-old with a well-functioning implant at 20 years post-surgery will be 75 — and may still need another 10 to 15 years of good joint function. This does not mean younger patients should not have knee replacements when they genuinely need them. It means the decision should be made with full awareness that a revision procedure may be needed in the future.
2. Patient Weight
Body weight places direct mechanical load on the knee replacement. For every kilogram of body weight, the force transmitted through the knee during walking is approximately three to four times that weight. A patient who is significantly overweight at the time of surgery places substantially higher stress on the implant, accelerating the wear of the bearing surfaces and increasing the risk of early loosening. Weight management before and after surgery is one of the most meaningful things a patient can do to extend implant life.
3. Activity Level and Type
Modern knee replacements are designed to withstand the demands of normal daily activity including walking, cycling, swimming, and light recreational activity. High-impact activities — running, jumping, heavy lifting, contact sports — accelerate bearing wear and are generally not recommended after total knee replacement. This is one of the facts that patients are sometimes not told clearly before surgery, particularly younger and more active patients who have specific sporting goals.
A knee replacement will change your life dramatically for the better if you have severe arthritis. It will not make your knee feel like a normal knee. Understanding this distinction before surgery leads to better satisfaction with the outcome.
4. Implant Design and Surgical Technique
Implant survivorship data consistently shows that modern implants from established manufacturers with long-term registry data outperform newer, less-documented designs. The surgical technique — specifically the alignment of the implant in the bone, the balance of the ligaments around the joint, and the handling of the surrounding soft tissues — has a profound effect on implant longevity and functional outcome. This is why surgeon experience and volume matter significantly for joint replacement.
5. Bone Quality
The implant is fixed to the bone with either cement or a press-fit porous coating that allows bone ingrowth. In patients with osteoporosis or poor bone quality, fixation is less reliable and the risk of loosening over time is higher. Bone density assessment before surgery helps identify patients who may need additional precautions.
What a Knee Replacement Can and Cannot Do
What It Reliably Delivers
• Significant and usually dramatic reduction in arthritic pain — this is the primary goal and it is achieved in over 90 percent of patients
• Restoration of the ability to walk, climb stairs, and perform daily activities without severe pain
• Correction of deformity — a knee that has bowed inward or outward from arthritis is realigned during the procedure
• Improved sleep quality — nighttime arthritic pain, which is particularly debilitating, resolves reliably after replacement
What It Does Not Deliver
• The feel of a normal knee — most patients describe their replaced knee as functional and comfortable but not identical to a natural joint. A minority of patients are aware of the implant during specific movements
• Full restoration of pre-arthritis activity levels — high-impact sport and heavy manual labour are restricted after replacement
• Guaranteed freedom from all knee discomfort — approximately 15 to 20 percent of patients report residual discomfort after knee replacement, though usually significantly less than pre-operatively
• Permanent solution — the implant will eventually wear and may require revision, particularly in younger patients
The Recovery Timeline — What Actually Happens Month by Month
• Days 1 to 3: In hospital. Standing and walking with a frame begin on the first day after surgery. Physiotherapy starts immediately.
• Week 1 to 2: Discharged home. Walking with crutches or a frame. Wound care and physiotherapy exercises at home.
• Week 2 to 6: Progressive increase in walking distance and independence. Driving typically resumes around six weeks for the right leg.
• Month 2 to 3: Most patients are walking without aids. Stairs are manageable. Swelling is gradually resolving.
• Month 3 to 6: Continued improvement in strength, flexibility, and endurance. Most daily activities are possible.
• Month 6 to 12: The final phase of recovery. The knee continues to improve in comfort and function. Full outcome is typically assessed at one year.
It is important for patients to know that the knee continues to improve for a full year after surgery. Patients who are disappointed with their progress at three months — which is still relatively early in the recovery — often find that months six through twelve bring significant additional improvement.
When Is Revision Knee Replacement Needed?
A revision knee replacement becomes necessary when the original implant fails. The most common causes of failure include aseptic loosening (the implant becomes loose from the bone without infection), bearing wear producing debris that causes bone loss (osteolysis), infection, instability, and stiffness. Revision knee replacement is a significantly more complex procedure than primary replacement and is performed by surgeons with specific revision experience. It carries higher complication rates and produces less predictable outcomes than primary replacement, which is one of the strongest arguments for optimising the conditions for longevity from the outset.
At Dr. Mandar Puranik’s joint replacement clinic in Kharadi, patients receive detailed pre-operative counselling that covers implant selection, activity modification, weight management advice, and long-term follow-up planning — all aimed at maximising the longevity of the replacement and the quality of the functional outcome.
Frequently Asked Questions
Q: Can I kneel after a knee replacement?
Kneeling is possible for most patients after knee replacement but is uncomfortable for many. The discomfort is usually from the incision scar and the changed sensation around the knee rather than pain from the implant itself. With practice, most patients can kneel for short periods. Prayer positions and tasks that require sustained kneeling are more challenging.
H3- Q: Can I have both knees replaced at the same time?
What It Does Not Deliver
Simultaneous bilateral knee replacement is performed in selected patients who are medically fit and have severe bilateral disease. It reduces the total recovery period compared to staged replacements but carries higher early risks of blood loss, medical complications, and rehabilitation demand. Dr. Mandar Puranik assesses each patient’s suitability for simultaneous replacement individually.
Q: What happens if my knee replacement gets infected?
Infection is the most feared complication of joint replacement. Depending on the timing and type of infection, treatment may involve antibiotics alone, surgical washout with implant retention, or complete removal of the implant with a staged revision. Prevention through meticulous surgical technique, antibiotic prophylaxis, and patient optimisation before surgery is far more important than treatment.
Q: How do I know when my knee replacement needs to be revised?
The typical symptoms of a failing knee replacement include new or worsening pain (particularly start-up pain after rest), instability, swelling, warmth, or increasing stiffness. Annual follow-up with X-rays at your joint replacement surgeon’s clinic allows early detection of loosening or wear before symptoms become severe.
A Knee Replacement Decision Deserves a Complete, Honest Conversation.
Dr. Mandar Puranik at Ortho Clinic Pune provides thorough pre-operative counselling so you know exactly what to expect before, during, and after surgery.
Visit orthoclinicpune.com or find us on Google to book your consultation today.
Ready to consult? Book An Appointment with Dr. Mandar Puranik today.
Google: Dr. Mandar Puranik on Google | Joint Replacement: Joint Replacement Surgery | About: About Dr. Mandar Puranik




